Scars: A guide to good healing
- Overview
Scars can be a source of anxiety for many people. You might be worried a scar isn’t healing fast enough, or that it looks worse than you think it should. Here’s how to help the process along and when to ask for help.
Keep an eye, not a hand on your scar
Monitoring your scar will help you to track its progress and catch any problems early, but you need to avoid touching the area unnecessarily. Do what you need to keep the area clean and dry, but make sure you sterilise your hands before applying any creams or gels that you have been advised to use. Never pick scabs, as this just prolongs the healing process and increases the risk of infection. Every scar is different so make sure you follow the specific advice given by your doctor.
The importance of keeping your wound clean cannot be understated. Infection is the worst thing for a healing scar. It will delay your healing and could make you very sick. Consult your GP if you notice any of the following signs:
- swelling, redness, itching and increasing pain in the affected area
- pus in or around the wound
- generally feeling unwell
- a raised temperature of 38C (100.4F) or above
- swollen glands in the chin, neck, armpits or groin.
Know your stage of recovery
Not knowing where you are in the healing process can lead to unnecessary concern or missing signs that the scar isn’t healing properly. If you have an incision or stitches, the wound can take a full three months to heal and the scar will fade over a number of years. Here’s how the process breaks down:
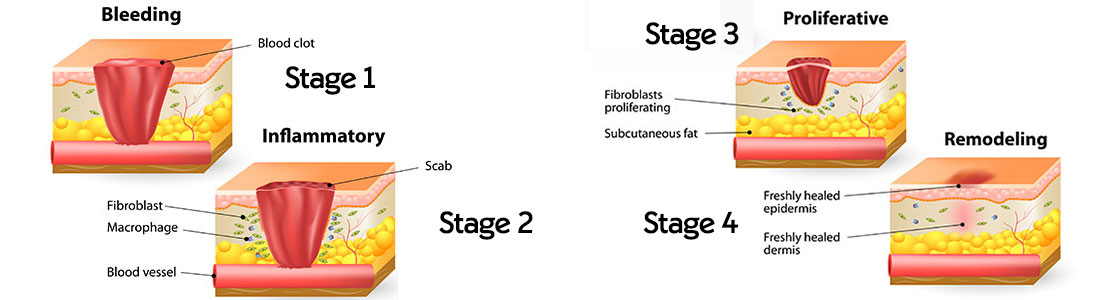
Stage one: Haemostasis
Blood rushes to the site of the wound and clotting occurs, stopping the bleed. This process begins immediately.
Stage two: Inflammation
Once haemostasis is achieved (usually within a few minutes) cells are sent to repair the wound. The wound heats up, pain increases, redness spreads. This can persist up to around day four.
Stage three: Proliferation
The tissue around the wound contracts, drawing the wound smaller and closing the skin. This usually occurs from around day four up to day 21.
Stage four: Remodelling
After around 21 days, the deeper structures begin to form, giving the wound tensile strength. This process can continue for around two years. It’s during this time that problems with the scar can occur and leave you with more severe scarring in the longer term.
Watch out for keloid and hypertrophic scars
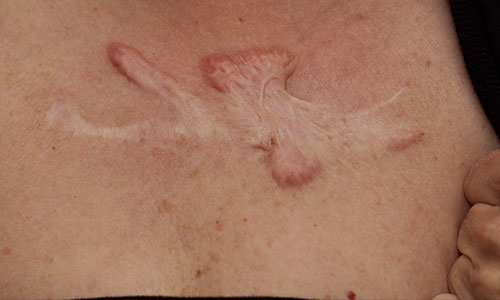
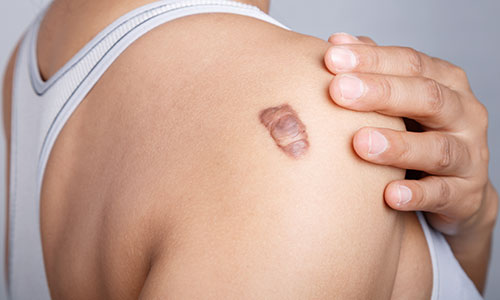

As connective tissue builds up during the remodelling phase, two key problems can occur – keloid and hypertrophic scarring.
In both keloid and hypertrophic scars the tissue continues to build up when the scar has effectively healed, causing it to darken and form large mounds of scar tissue. They look similar, but have very different outcomes. Keloids are difficult to treat and will never improve on their own while hypertrophic scars may fade with time and respond well to steroid treatment.
Telling the difference is hard, so if you think a keloid or hypertrophic scar is forming or you have had keloids before, let your GP or skin specialist know as soon as possible. Early steroid treatment may reduce risk of developing a keloid scar but once it has formed there are limited ways to improve its appearance. There are options such as cryosurgery, excision, laser and steroid injections that can be explored, but there can be a risk of further scarring.
Keloids are fairly rare, occurring in just 10% of people. They’re more common in those of Afro-Caribbean decent or with darker skin and are more likely to occur on the shoulders, face, upper chest and back. If you’ve had a keloid before your risk of having another is heightened.
Hypertrophic scars won’t grow as large as keloids and may fade on their own. However, they are more common in all racial groups. Hypertrophic scars usually respond well and flatten out with steroid treatment. Silicone tape has also been seen to be an effective treatment for hypertrophic scars.
Click here for more information about options for serious scars and burns.
Healthy skin, healthy scars
The best way to improve your chances of a good outcome is to start with healthy skin. Vitamin C, E, zinc and B are all very good for the skin and I have seen particularly good results with the use of vitamin A – not just in creams but in your diet (WARNING: don’t use vitamin A if you are pregnant).
Make sure you get plenty of these vitamins while healing, and keep your scar out of the sun, which can cause pigmentation issues, including melanoma.
Last updated Monday 14 June 2021
First published on Thursday 29 September 2016


