Your guide to the pelvic floor
- Overview
What do pelvic floor muscles do?
Pelvic floor muscles support and protect your pelvic organs – the bladder, bowel and uterus – especially when standing.
Strong pelvic floor muscles lead to increased sensitivity during sex and stronger orgasms, as well as preventing your bowel and bladder from leaking.
Where are the pelvic floor muscles?
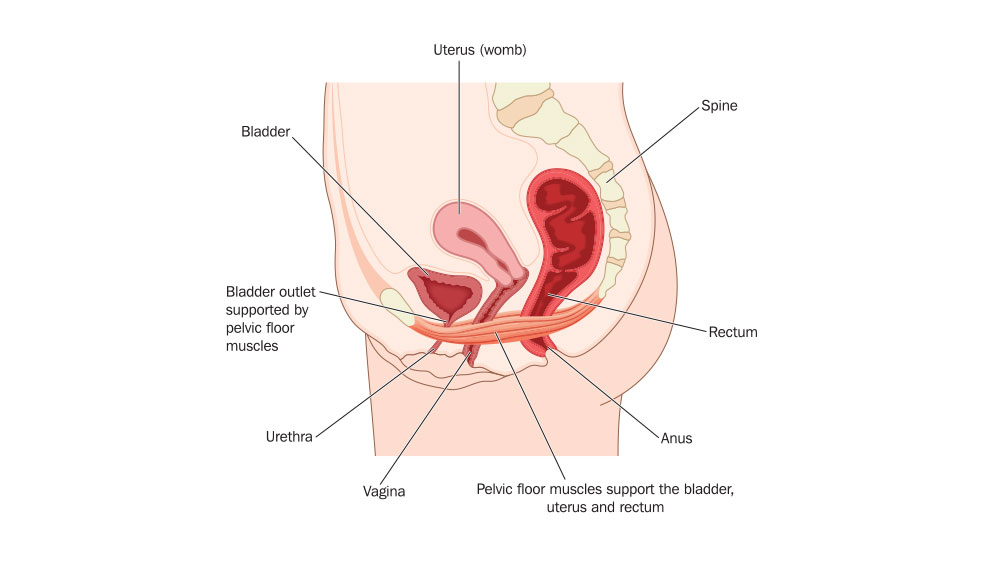
The pelvic floor muscles run between the legs from the pubic bone to the tailbone. They’re a supportive ‘hammock’ of muscles that line the pelvis and are made up of superficial and deep layers.
It can be difficult to locate and contract your pelvic floor muscles at first. Speaking to a specialist pelvic health physiotherapist can be useful.
It can also be helpful to imagine you’re trying to stop yourself from passing urine or wind by squeezing and lifting the muscles upwards and forward towards your pubic bone.
Why should I train my pelvic floor muscles?
Like other muscles, your pelvic floor muscles benefit from regular exercise.
Weak pelvic floor muscles are quite common – in fact, 1 in 3 women will experience problems with their pelvic floor muscles at some point during their lives.
This weakness may lead to:
- leaking urine when running, jumping, coughing, laughing or sneezing (stress incontinence)
- leaking urine after a sudden urge to pass urine (urge incontinence)
- a combination of the above (mixed incontinence)
- stool leakage
- decreased sensitivity during sex
- an increased risk of developing pelvic organ prolapse, which may need surgery.
Can strengthening the pelvic floor muscles help incontinence?
Strengthening your pelvic floor muscles can improve and cure incontinence.
Stress incontinence usually happens when the muscles used to prevent urination are weak or damaged, which can be caused by:
- pregnancy/childbirth
- a long-term cough
- constipation
- being overweight
- ageing/menopausal changes
- pelvic surgery or trauma
- repeated heavy lifting
- high-impact exercise.
The good news is, you can strengthen pelvic floor muscles like any other muscles with simple, regular exercise.
Should I perform pelvic floor exercises during pregnancy?
Absolutely – starting a pelvic floor strengthening programme from early pregnancy is completely safe.
During pregnancy greater strain is placed upon your pelvic floor muscles and, regardless of whether you have a vaginal delivery or caesarean section, these muscles will need targeted strengthening to help reduce or avoid stress incontinence after pregnancy. It's never too late to start, but starting them early will help.
Exercises to strengthen the pelvic floor muscles
Pelvic floor exercises can strengthen the muscles around your bladder, vagina and back passage.
We recommend you seek advice from a specialist pelvic health physiotherapist to help with your exercise programme. They can ensure you’re doing the exercises correctly and create a personalised plan for you. Many women also find regular contact with a physiotherapist motivating – similar to the reasons why many people use a personal trainer, for example.
For your complete reassurance, Nuffield Health physiotherapists follow the NICE Guidelines for Urinary Incontinence. For women with stress or mixed incontinence, they recommend a program of supervised pelvic floor muscle training with a specialist physiotherapist for at least three months.
If you’re having trouble contracting your pelvic floor muscles during your physiotherapy session, your physiotherapist might suggest using electrical stimulation. Pelvic floor muscle toners, educators and vaginal weights can also help you get started and stay on track.
Exercises for the pelvic floor muscles include long and short squeezes. Try and aim for:
- 10 long squeezes, held for 10 seconds each
- 10 short squeezes, held for 1 second each.
Are there pelvic floor exercises for men too?
Yes – men can also benefit from strengthening their pelvic floor. Pelvic floor dysfunction in men can manifest as:
- urinary stress incontinence
- erectile dysfunction
- premature ejaculation
- a post micturition dribble.
Pelvic issues in men can be due to general weakness in the pelvic floor muscles. Prostate surgery may also affect the pelvic floor and its delicate nerve supply.
A pelvic health assessment and targeted exercises similar to those above can help.
Creating a routine
Remembering to exercise your pelvic floor muscles can be tricky. So, try making the exercises part of your routine using triggers and prompts:
- Place sticky notes in places where they’ll catch your eye, e.g. on the fridge or kettle
- Set alarms on your watch/phone
- Download specific apps on your phone – we recommend the Squeezy app
- Exercise after you’ve been to the toilet, or while you’re waiting for the kettle to boil or washing your hands.
Strong pelvic floor muscles can significantly improve your quality of life

It’s worth working with a physiotherapist and persevering with your programme – pelvic floor muscle physiotherapy helps cure or improve the symptoms of weak pelvic floor muscles for over 70% of women. It can also help you recover from pelvic prolapse surgery and other women’s health issues.
Like more advice or support? Get in touch with one of our specialist pelvic health physiotherapists.
Last updated Friday 5 May 2023
First published on Wednesday 11 March 2020

