Mammogram (breast screening)
- Overview
Or call us on
Reviewed by Danielle Nixon (Radiology Manager) and Lisa Serevena (Quality Lead Diagnostic Radiology)
A mammogram is a diagnostic test used to look for any problems within the breast and surrounding tissues. At Nuffield Health some women are eligible to refer themselves for self-pay breast screening.
What is a mammogram?
A mammogram is used to look for any problems within the breast and surrounding tissues. It uses X-rays to find cancers in the breast which are too small to feel.
How will I know if I need a screening mammogram?
Breast screening is suitable for women over 40 years of age who have no breast symptoms and who have not had a mammogram within the last 12 months. Women with concerns about possible breast cancer symptoms should book an appointment with a GP or consultant.
The purpose of breast screening mammograms is to find breast cancer early. This promotes early diagnosis and simpler treatment.
The risk of developing breast cancer increases with age with most cancers found in women over the age of 50. A small number of breast cancers are caused by genetic mutations and are found within family groups; however, lifestyle factors can also impact risk. Being overweight, drinking alcohol and smoking can all increase a person’s risk of developing breast cancer.
How can I book a mammogram?
To book a screening mammogram, call us on 0345 230 2040. You can refer yourself for a self-pay mammogram if you're over 40 years old and haven't experienced any symptoms or had screening within the last 12 months.
How should I prepare for a mammogram?
Before your appointment, you will need to ensure that you have told us if you have had a previous mammogram. It is important that we have this information available when your screening mammogram is reported. Please also let the team know when you book if you have breast implants.
Please do not use deodorant or talc on the day of your examination, as this can cause artefact on the imaging.
What happens during a mammogram?
After undressing to your waist, the mammographer will position you next to the X-ray machine and will place each of your breasts in turn onto the X-ray table, compressing them firmly with a plastic plate while the picture is taken. This takes only a few seconds and then the pressure is released. At least two views are taken on each side to show all the breast tissue.
It may be uncomfortable and, very rarely, it may be painful. If you do experience discomfort or pain, please tell your mammographer right away and they will do what they can to make you more comfortable.
How long does a mammogram take?
The whole examination should take no more than 15 minutes and you will be able to leave the hospital straight after your appointment.
How/when will I receive my results?
You will receive your results within two weeks of your appointment. If your result is abnormal, this will be discussed with you by a doctor.
What do the results mean?
Statistics show that 96% of women will receive a normal mammogram result. In around 4% of cases, mammograms need to be repeated for technical reasons, for example, if you were not in the correct position or moved slightly during the picture.
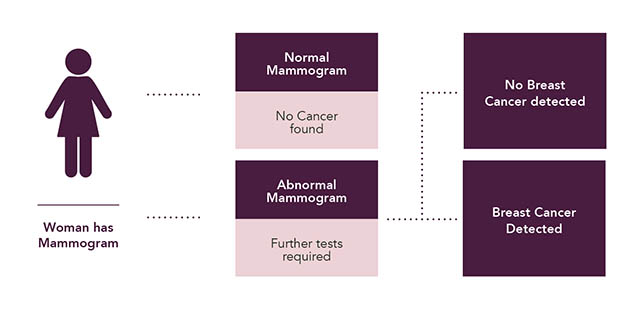
It is not always easy to diagnose breast cancer on a mammogram and some women will receive a false positive result. We understand that this can be a worrying time and, following a positive result, further tests will be completed to provide confirmation.
It is also possible to be given a normal result when a small cancer is there as not all cancers are visible on a mammogram. This is called a false-negative result. Therefore, even after a normal breast screening, you should always see your GP if you find a change in your breast. Statistics show that there is a likelihood of one cancer being missed when 2,500 women are screened so this is very rare.
Ways to pay
Nuffield Health promise
Our prices are all-inclusive. We will equal any comparable price. There are no time limits on your aftercare.
Paying for yourself
There are no hidden costs in our treatment prices. The price you see is the price you pay.
Find out morePersonal medical loan
Spread the cost of your treatment with a 10, 12 or 24 month 0% personal medical loan.
Find out moreMedical insurance
We work with you and your insurance provider to get you the treatment you need quickly
Find out more